G8 Nexum -
The Complete
HMO Operating
System
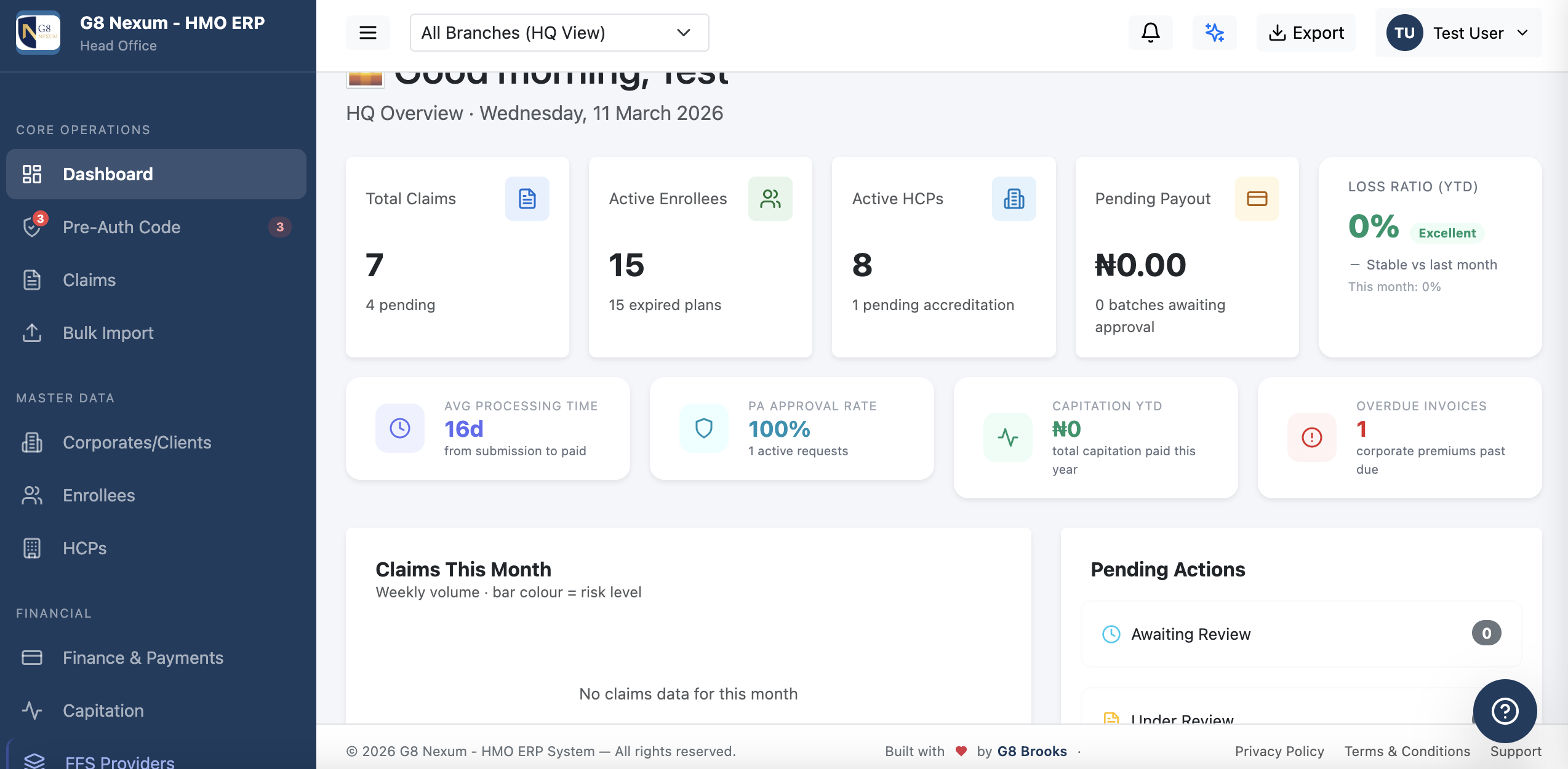
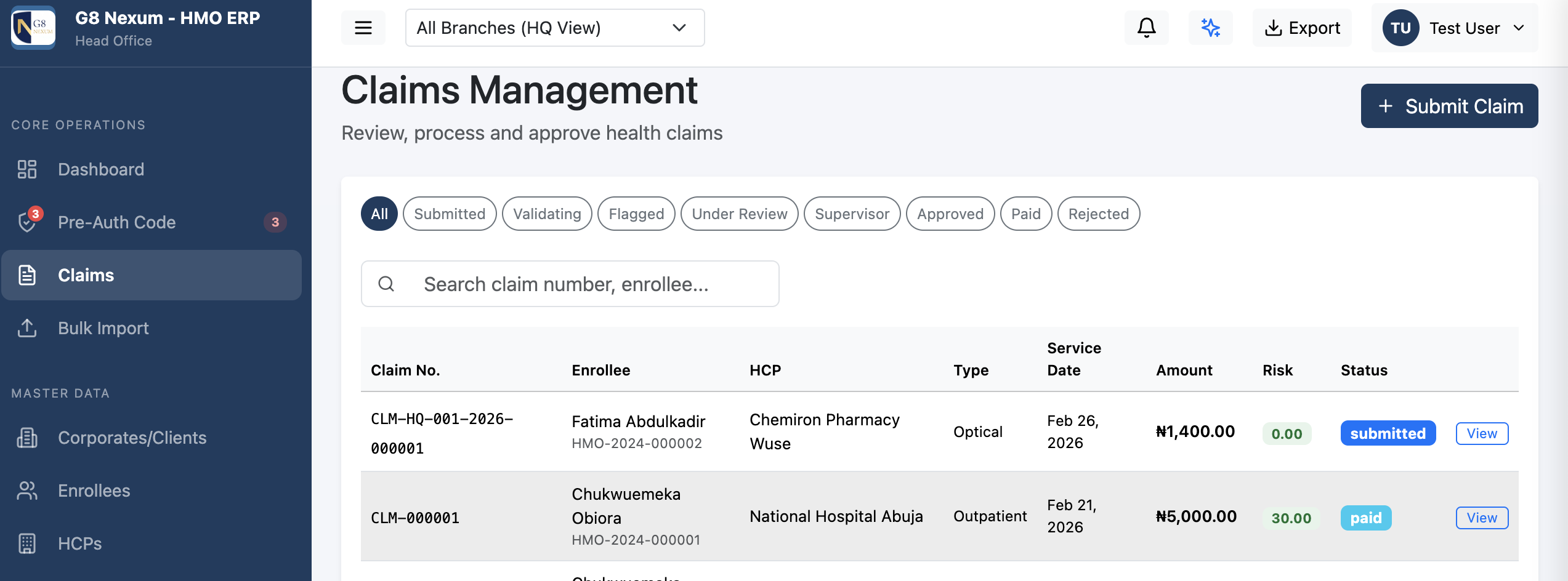
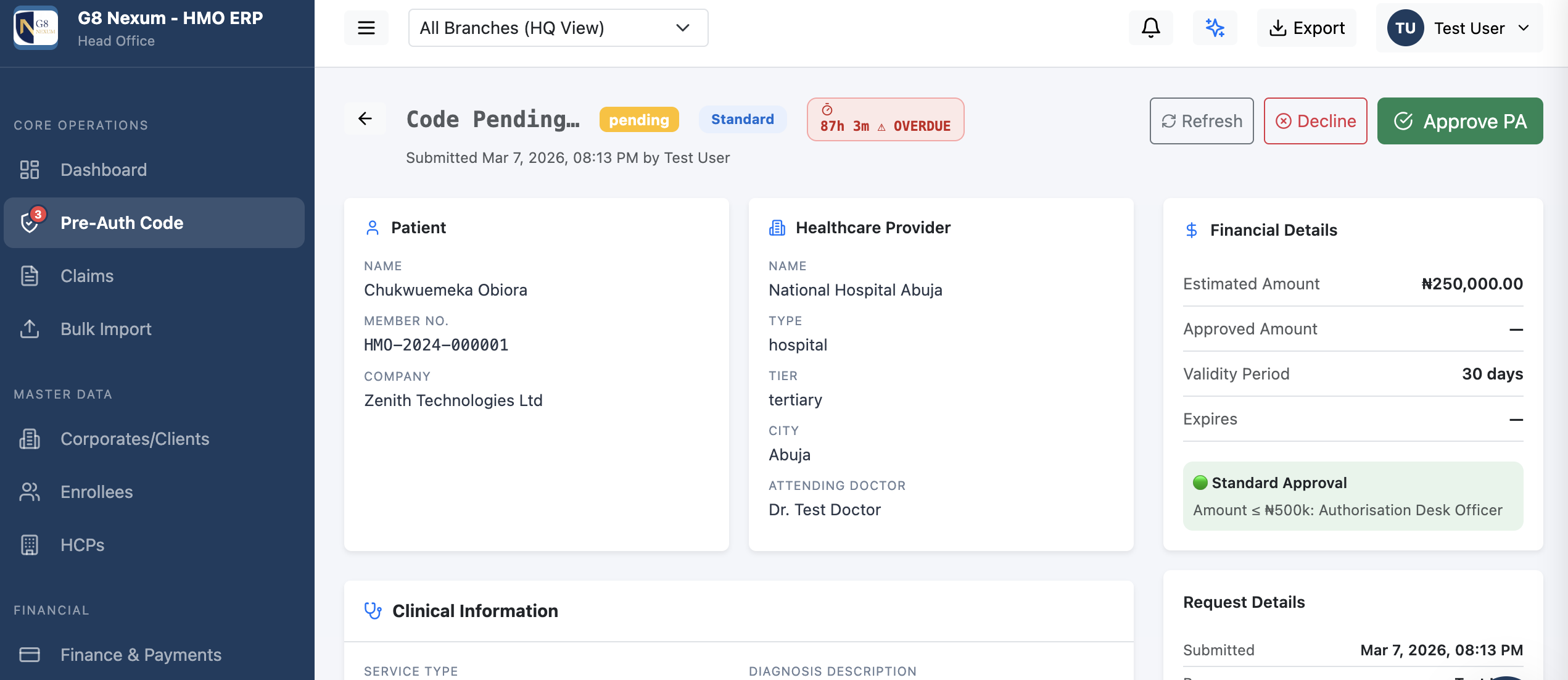
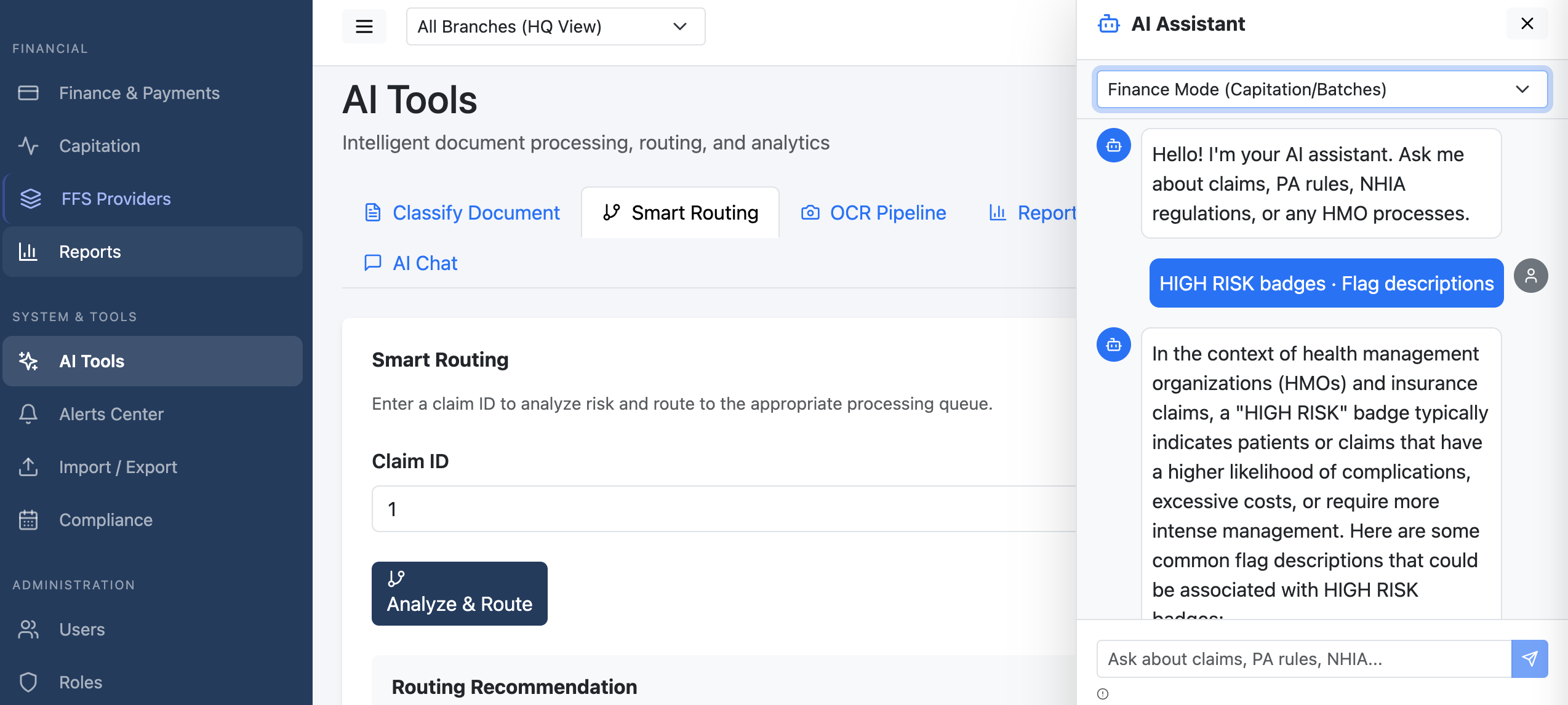
G8 Nexum gives your HMO one platform to run everything - claims, pre-auth, capitation, fraud detection, finance, and AI. Purpose-built for Nigerian health insurance operations.